
Introduction
A patient calls your healthcare support center, confused about their insurance coverage for an upcoming specialist visit. Your agent needs to verify plan status, check referral requirements, confirm pre-authorization protocols, and stay HIPAA-compliant — all while the patient waits on hold.
One incorrect answer about coverage can result in a denied claim, a regulatory penalty, or broken patient trust.
Healthcare contact centers handle the highest-stakes interactions of any industry. Yet agents are often left relying on memory, scattered policy documents, or supervisor escalations.
Agent errors account for 38% of calls not resolved on first contact. In healthcare, those errors carry compliance and patient safety consequences that go far beyond a frustrated caller. Decision trees exist to close that gap — here's how they work and why they matter.
What Is a Healthcare Decision Tree for Contact Center Agents?
A healthcare decision tree is an interactive, branching workflow that guides agents through complex patient queries step by step. At each node, the agent asks the patient a specific question, and based on the answer, the tree routes them to the next appropriate action — until they reach a resolution, escalation trigger, or compliance-approved script.
That distinction matters. Clinical decision trees support treatment planning; contact center decision trees are operational tools built for administrative processes — insurance verification, billing disputes, prior authorization requests, and pharmacy benefit inquiries.
Core Structural Components
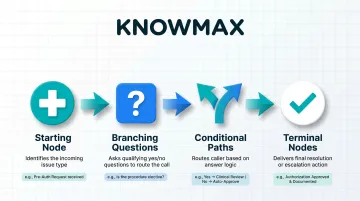
Each decision tree contains:
- Starting node: The patient's issue category (e.g., "pre-authorization request")
- Branching questions: Binary or multiple-choice prompts answerable with information the agent can confirm during the call
- Conditional paths: Routes that adapt based on patient-specific variables like plan type, coverage status, or service requirements
- Terminal nodes: Resolution actions, pre-approved scripts, documentation requirements, or escalation instructions
In healthcare, this structure matters because queries involving protected health information (PHI), insurance coverage, prescriptions, or billing follow strict regulatory and procedural rules. A decision tree encodes those rules directly into the workflow — so agents aren't memorizing compliance requirements, they're just following the next prompt. That's what prevents errors like unauthorized PHI disclosure or a missed pre-auth step that triggers a claim denial.
Why Healthcare Agents Struggle Without Decision Trees
Healthcare contact center agents must navigate insurance plan types, referral workflows, pharmacy benefit structures, billing codes, and HIPAA privacy regulations — often within a single call. That knowledge is scattered across disconnected SOPs, training manuals, and undocumented institutional expertise. Recalling it consistently under call pressure is unrealistic without structured support.
The Knowledge Complexity Problem
In healthcare payer contact centers, 40% of call time on benefit inquiries is spent as "dead air" — prolonged silence or hold time while the agent searches across 7-11 different systems. Each benefit inquiry requires 12+ steps and 15+ clicks to resolve, and 25% of these calls require a customer callback.
Without structured guidance, agents face:
- Scattered knowledge across multiple platforms
- Policy nuances that vary by plan type, region, and service category
- Constantly changing formularies, coverage rules, and authorization requirements
- High cognitive load managing compliance protocols alongside resolution steps
The Compounding Cost of Errors
In healthcare, incorrect information has severe consequences. Since April 2003, the Office for Civil Rights has received 374,321 HIPAA complaints, with 152 cases resulting in financial settlements totalling $144,878,972. The top compliance issue: impermissible uses and disclosures of PHI.
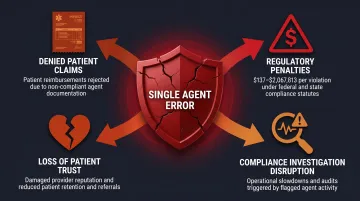
A single agent misstep — failing to verify caller identity, discussing PHI in an unsecured environment, or providing incorrect coverage information — can trigger:
- Denied claims for patients
- Regulatory penalties ranging from $137 to $2,067,813 per violation tier
- Loss of patient trust
- Operational disruption from compliance investigations
The downstream impact compounds fast. 86% of claim denials are avoidable, and the top cause is missing or inaccurate data (50%). A significant share of these denials trace back to incorrect information provided during the initial patient interaction.
The Agent Onboarding Challenge
Healthcare payer contact centers require 6 to 9 months to fully train a new agent, compared to 4-10 weeks across general industries. One large healthcare insurer reported an 18-week baseline training program just for call center and claims roles.
This extended timeline reflects just how complex healthcare queries are — not just procedurally, but regulatorily. Without structured guidance built into the workflow, new agents spend months dependent on supervisors for calls they should be handling independently. Decision trees change that by embedding the right guidance at the point of need, not just during training.
Key Use Cases: How Decision Trees Guide Healthcare Agents
Healthcare contact centers handle the same complex query types, call after call — insurance authorizations, referrals, prescriptions, billing disputes. Decision trees map these scenarios into step-by-step workflows, so agents follow a consistent path instead of relying on memory or judgment under pressure.
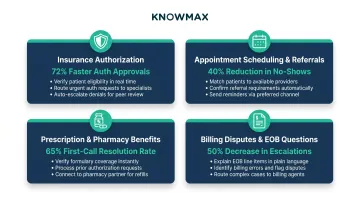
Handling Insurance Authorization and Coverage Queries
Insurance authorization queries are the #1 call driver in healthcare payer contact centers, accounting for 50-60% of all inquiry calls. Agents must navigate plan-specific rules, coverage tiers, and authorization requirements that vary by service type and provider network.
A decision tree walks agents through eligibility verification steps:
- Is the patient's plan active?
- Does the requested service require pre-authorization?
- What is the in-network vs. out-of-network distinction for this plan?
- What documentation needs to be collected from the provider?
Each answer routes the agent to the next step based on confirmed patient details, ensuring accurate coverage determinations without relying on memory. Physicians spend an average of 13 hours per week completing prior authorizations, and 93% report that PA delays access to necessary care. Decision trees reduce this burden by giving agents a clear, step-by-step path through the authorization workflow — cutting confusion and speeding up each interaction.
Managing Appointment Scheduling and Referral Requests
Referral workflows involve multiple dependencies: Does the patient's plan require a PCP referral? Is the specialist in-network? Does the referral need insurer approval before the appointment can be scheduled?
Branching logic handles this complexity:
- Verify plan type and referral requirements
- Confirm specialist network status
- Check if pre-authorization is needed
- Provide next steps for the patient (e.g., contact PCP, wait for approval)
This ensures agents give accurate guidance without needing to memorize the full policy rules for every plan type.
Answering Prescription and Pharmacy Benefit Inquiries
Medication and pharmacy benefit questions come up constantly in healthcare contact centers. Agents must determine:
- Is the drug on the formulary?
- Which tier is it classified under?
- Are there prior authorization requirements?
- Is a generic substitute covered, and what is the patient's expected cost-share?
Decision trees guide agents through these questions in sequence, helping them deliver accurate answers without toggling between multiple disconnected systems or pharmacy benefit management platforms.
Resolving Billing Disputes and Explanation of Benefits (EOB) Questions
79% of consumers have been surprised by the price of a medical bill, and 39% cite difficulty understanding insurance coverage or denials. Billing queries are complex — agents must sort through several variables before they can give a patient a clear answer.
A decision tree helps agents determine:
- Was the claim denied or underpaid?
- Was the provider in-network at the time of service?
- Was the service pre-authorized as required by the plan?
- Is this a billing error, a plan exclusion, or a patient responsibility issue?
Each path ends at a specific resolution action — whether that's initiating a claims review, flagging a billing error, or escalating to a supervisor — so no call ends with a vague "I'll look into it."
How to Build an Effective Healthcare Decision Tree
Building decision trees that agents will actually use requires a methodical approach focused on real-world query patterns and ongoing maintenance.
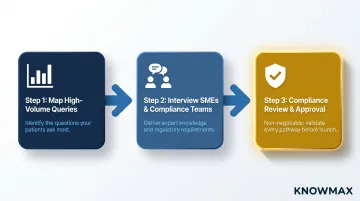
Step 1 — Map Your Highest-Volume, Highest-Error Query Types First
Don't attempt to build every possible workflow at once. Start by auditing:
- Call recordings and ticket data to identify the 5-10 query types generating the most repeat contacts
- Escalation logs to pinpoint queries with the longest handling times or most frequent errors
- Agent feedback on which queries cause the most confusion or require supervisor assistance
These high-impact queries should be your first decision trees. For most healthcare contact centers, this includes insurance authorization, appointment scheduling, prescription coverage, and billing disputes.
Step 2 — Interview Subject Matter Experts and Compliance Teams
The logic within each tree must reflect both operational workflows and regulatory requirements. Schedule structured interviews with:
- SMEs who can surface edge cases, plan-specific nuances, and resolution steps that training documents typically miss
- Compliance teams who can verify the tree meets HIPAA data handling protocols, CMS guidelines, and applicable state-specific regulations
Compliance review is non-negotiable. The tree must script out PHI verification steps, secure communication protocols, and approved language for coverage determinations.
Platforms like Knowmax include authorization workflows that allow compliance teams to review and approve decision tree content through a maker-checker process before it's published to agents, ensuring regulatory alignment from the start.
Step 3 — Write Questions in Plain, Answerable Language
Every branching question must be answerable with information the agent can confirm during the call. Avoid internal jargon, system codes, or ambiguous phrasing.
Good example: "Is the patient's insurance plan still active as of today's date?"
Bad example: "Verify eligibility status per system code 247."
Answer options should be binary or limited-choice where possible, and clearly distinct with no overlap, so agents never get stuck choosing between two valid paths. If a question has more than four answer options, consider breaking it into multiple sequential questions.
Step 4 — Test with Agents Before Deployment
Walk through the tree using real or simulated call scenarios with agents who were not involved in building it. Gaps, confusing branches, or dead ends will surface immediately.
Track where agents:
- Hesitate or ask clarifying questions
- Choose the wrong path
- Request supervisor assistance despite following the tree
- Report that the final resolution doesn't match the patient's actual issue
Each of these signals a specific branch that needs reworking. Run at least two rounds of testing — the tree is ready when agents can reach the correct resolution on first attempt without escalating.
Step 5 — Build for Ongoing Maintenance
Healthcare regulations, plan structures, and formularies change frequently. The decision tree must be treated as a living document with:
- Assigned ownership: Designate a specific team or role responsible for updates
- Review cadence: Tie reviews to policy change cycles (e.g., quarterly plan updates, annual formulary changes)
- Version history: Track changes to ensure agents are always using the current workflow
Knowmax's decision tree builder includes scheduling and archiving features that let teams set start and end dates for content availability. Outdated workflows are automatically retired, so agents always access the current guidance without manual intervention.
Benefits of Healthcare Decision Trees for Contact Centers
Reduced Agent Errors and Compliance Risk
When agents follow a verified, step-by-step guided path, the chance of providing incorrect information drops significantly. Decision trees ensure that every PHI-handling protocol, pre-authorization requirement, and coverage determination is executed consistently.
Healthcare contact centers achieve an average first-call resolution rate of just 52%, meaning nearly half of patients must call multiple times. The agent is the primary source of error in 44% of unresolved calls. Decision trees address this by eliminating reliance on memory and scattered knowledge sources.
Faster Resolution and Lower Average Handle Time
Decision trees eliminate the time agents spend searching for answers mid-call. Every response surfaces the next step immediately, compressing resolution time and reducing the need for holds or supervisor escalations.
Average handle time in healthcare contact centers is 6.6 minutes, with 40% of benefit inquiry time spent in dead air while agents search across systems. One general contact center achieved a 30% AHT reduction within 12 weeks using guided workflows and high-quality knowledge bases, cutting search time by 60–90 seconds on complex calls.
Accelerated Onboarding for New Agents
New hires don't need to internalize complex policy documents before handling calls independently. The decision tree carries them through correct processes from day one, reducing the ramp-up period and allowing teams to scale reliably during hiring surges.
The results across healthcare and adjacent industries are consistent:
- One large healthcare insurer cut onboarding cycle time by 15% from an 18-week baseline, saving several million dollars annually
- A general BPO contact center reduced time-to-proficiency by 75% — from 60 days to 15 days — using guided knowledge workflows
Integrated Guidance at the Moment of Need
Knowmax delivers HIPAA-compliant, interactive decision trees that surface directly on the agent desktop — no tab-switching, no manual lookups. It integrates with Salesforce, Zendesk, Genesys, Freshdesk, and Talkdesk, so guidance appears at the exact moment it's needed.
The decision tree module includes:
- Multimedia nodes and pre-approved compliance scripts for consistent patient communication
- PHI-handling instructions and escalation triggers built into each workflow
- Role-based access controls so agents only see what's relevant to their role
- Maker-checker approval workflows so compliance teams can review content before it goes live
Frequently Asked Questions
What is a decision tree in healthcare?
In healthcare, decision trees have two primary uses: clinical decision trees model treatment pathways and health economics, while agent-guidance decision trees walk contact center agents step-by-step through administrative queries like insurance authorization, billing disputes, and pharmacy benefit inquiries. The two serve very different purposes — this guide covers the agent-guidance type.
How are decision trees used in healthcare?
In contact centers, decision trees give agents a structured path through complex queries. Common use cases include insurance coverage verification, appointment scheduling, referral workflows, prescription inquiries, and billing dispute resolution — each guided by branching yes/no or multiple-choice steps until the query is resolved.
For which scenario would the use of a decision tree be most appropriate?
Decision trees work best when a query has multiple possible paths based on patient-specific variables — plan type, coverage status, authorization requirements. They're especially valuable when taking the wrong path carries compliance or patient-experience consequences, such as in pre-authorization requests and billing dispute resolution.
What is decision tree analysis with an example?
Decision tree analysis breaks a complex process into sequential binary or multiple-choice questions. For a pre-authorization query, an agent works through: Is the plan active? → Is the service covered? → Is prior auth required? → What documentation is needed? Each answer drives the next step until resolution.
What are the four types of decision trees?
The four common types are binary trees (yes/no branching), multi-way split trees (multiple-choice paths), classification trees (which sort queries into outcome categories), and regression trees (used to predict numerical results). For contact center work, binary and multi-way split trees are the standard — they map cleanly to how agents navigate patient queries step by step.


