
Introduction
Healthcare contact centers face mounting pressure. Call volumes surge unpredictably, staff turnover hovers near 40%, and patients abandon calls after waiting just over a minute.
When patients do connect, nearly half of their interactions fail to resolve on the first try—forcing callbacks that compound operational costs and erode satisfaction.
First-call resolution (FCR) captures this failure most starkly. SQM Group benchmarks show healthcare contact centers average 71% FCR, well below the 80% world-class threshold that only 4% of centers achieve.
Every unresolved call triggers a cascade: patient frustration climbs, agents burn out faster, and operating costs balloon. Research shows member satisfaction drops 15% with each callback, and patients who experience negative phone interactions are four times more likely to switch providers.
AI agents are changing this equation. By routing calls intelligently, surfacing knowledge in real time, automating routine requests, and escalating based on sentiment, AI-powered contact centers are closing the FCR gap. This article breaks down what FCR means in healthcare, why it consistently underperforms, and exactly how AI agents improve resolution rates—with specific mechanisms, not surface-level claims.
TLDR
- Healthcare contact centres average 71% FCR, falling short of the 80% world-class benchmark
- AI agents lift FCR through smart routing, real-time knowledge delivery, self-service automation, and sentiment-aware escalation
- Every 1% FCR gain saves roughly $286,000 annually and improves patient satisfaction by 1%
- Autonomous agents handle routine calls; agent-assist tools support agents on complex interactions — each type serves a distinct role
- Effective FCR measurement combines ACD data, post-call surveys, and AI conversation analytics
What Is First-Call Resolution in Healthcare—and Why Does It Matter?
First-call resolution measures the percentage of patient calls fully resolved during the first interaction, with no transfer, callback, or escalation required. The formula is straightforward: (calls resolved on first contact ÷ total calls) × 100.
In healthcare, "resolved" spans a wide scope—appointment scheduling, billing disputes, insurance coverage questions, referral status updates, prescription refills, and clinical inquiries. Each requires accurate information delivered quickly, often while agents toggle between EHR systems, CRMs, and scheduling platforms.
FCR Benchmarks in Healthcare
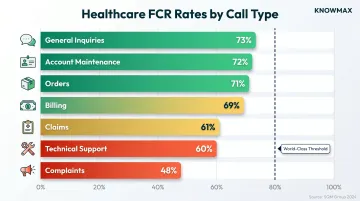
Industry data reveals stark variation in FCR performance by call type and channel:
| Call Type | FCR Rate |
|---|---|
| General Inquiries | 73% |
| Account Maintenance | 72% |
| Orders | 71% |
| Billing | 69% |
| Claims | 61% |
| Technical Support | 60% |
| Complaints | 48% |
Source: SQM Group 2024
Claims and complaints—two high-volume healthcare categories—show the lowest resolution rates, indicating structural complexity that standard agent workflows struggle to address.
Why FCR Matters More in Healthcare
FCR directly influences value-based reimbursement. Peer-reviewed research published in the American Journal of Managed Care found that call center speed-to-answer inversely correlates with patient perceptions of access and timeliness—metrics captured in HCAHPS surveys that affect Medicare reimbursement rates.
The financial stakes are just as concrete. Every 1% FCR improvement generates approximately $286,000 in annual savings for the average healthcare insurance call center.
Patient retention compounds that figure further. 95% of customers continue doing business with an organization when their issue is resolved on first contact. With the average patient generating roughly $12,000 in lifetime value, a single poor contact center experience carries direct revenue consequences—not just a satisfaction score.
Why Healthcare Contact Centers Fail to Resolve Calls on the First Try
Knowledge and Context Gaps
Agents frequently lack real-time access to patient history, EHR data, or current policy details during live calls. McKinsey reports that 30% to 40% of claims call handling time is unproductive "dead air" while agents search for information across disconnected systems.
Switching between EHR platforms, scheduling tools, and CRMs costs 30 to 60 seconds per call — time that compounds across thousands of daily interactions. Without unified desktops or AI-powered knowledge surfacing, agents spend more time searching than solving, driving up handle times, incorrect answers, and patient callbacks.
Transfer Chains and Misrouting
A call that bounces from scheduling to billing to clinical departments often loses context entirely. Each transfer resets the patient's narrative, increases abandonment risk, and reduces resolution likelihood. Transfer rates in healthcare reach 19%, and a single transfer reduces patient satisfaction ratings by 12%.
Misrouting stems from legacy IVR systems that rely on rigid menu trees rather than understanding patient intent. When a patient selects "billing" but actually needs a referral status update, the system routes them to the wrong team — and the resolution clock resets before the conversation even begins.
Structural Challenges Unique to Healthcare
Healthcare contact centers experience 30% to 40% annual agent turnover—the highest of any industry vertical. Attrition costs $10,000 to $20,000 per agent in recruiting, training, and lost productivity. High turnover creates a perpetual knowledge gap, as newer agents lack the institutional expertise required to navigate complex patient scenarios confidently.
Call abandonment rates average 7%, with 60% of patients abandoning if wait times exceed one minute. Staffing shortages exacerbate this: typical healthcare contact centers meet only 60% of required peak coverage, leaving an average of 23 agents short during busy periods.
Multilingual patient populations add another layer of complexity. 25.7 million people in the US have limited English proficiency (LEP), with 4.9 million enrolled in Medicaid or CHIP. The top languages among LEP individuals include:
- Spanish — 63%
- Chinese — 7%
- Vietnamese — 3%
- Arabic — 2%
- Tagalog — 2%
HHS Section 1557 mandates qualified interpreter services, but staffing multilingual agents around the clock remains operationally difficult for most contact centers.
How AI Agents Improve First-Call Resolution in Healthcare Contact Centers
Intelligent Call Routing and Intent Classification
AI-powered routing analyzes patient intent using natural language processing before the interaction reaches a human agent, or resolves it autonomously. Unlike static IVR menus, AI routing identifies the specific purpose (prescription refill, appointment change, billing dispute, referral status) and directs the call to the optimal workflow with full context intact.
The right first touchpoint means resolution happens in a single interaction. Summa Health deployed Hyro's AI platform and achieved 76% successful AI call routing with 98% accuracy, deflecting repetitive inquiries that previously accounted for 20% of total call volume. The system engaged 85% of callers and reduced the burden on human agents, allowing them to focus on complex cases requiring empathy and judgment.
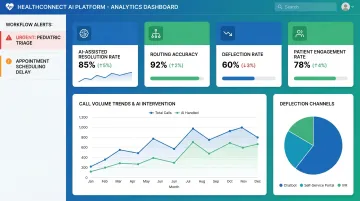
Prisma Health achieved an 80% chat resolution rate using AI agents for provider search, appointment management, and scheduling. The deployment generated over $300,000 in annual savings during the first year while maintaining a 67% engagement rate and 66% self-service reschedule rate.
These outcomes contrast sharply with legacy systems. McKinsey found that only 10% of current conversational AI interactions fully resolve without human handoff, underscoring the importance of deploying intelligent routing paired with escalation protocols rather than treating AI as a wholesale agent replacement.
Real-Time Knowledge Surfacing for Agent Guidance
Even when a human agent handles a call, their ability to resolve it on first contact depends on how quickly they can access the right information. AI-powered knowledge management platforms surface step-by-step resolution paths, decision trees, and policy content mid-conversation, reducing handle time and error rates.
Knowmax's platform exemplifies this approach, with capabilities built specifically for high-stakes contact center environments:
- AI-powered search understands natural language queries, delivering real-time answers from medical literature, organizational protocols, and knowledge bases without leaving the interaction interface
- Interactive decision trees guide agents through complex workflows (prior authorizations, post-care navigation, scheduling exceptions), ensuring compliance even for newer staff
- Visual how-to guides break down complex problems into clear steps, minimizing explanation time
- Role-based access control ensures agents see only information relevant to their function, improving security and focus
- Real-time content updates distribute time-sensitive care information instantly across teams, so agents always work from current protocols
The consistency this creates is particularly valuable in healthcare. Every agent, regardless of tenure or shift, accesses the same verified knowledge — narrowing the performance gap between best and worst on the floor.
Outdated information about coverage, referral processes, or appointment protocols is one of the most common triggers for patient callbacks. Centralized, AI-managed content updates eliminate that gap entirely.
Automated Self-Service for High-Volume Routine Requests
AI agents handle end-to-end resolution for high-frequency, low-complexity healthcare call types: appointment scheduling, prescription refill requests, bill balance inquiries, clinic hours, and referral status updates. Calls regarding claims and finding care account for 50% to 70% of payer call volume, with billing errors generating an additional 10% to 15%.
Autonomous resolution of routine calls reduces queue pressure on human agents. That frees agents to give fuller attention to complex or sensitive cases, improving FCR rates for those interactions too. Automating 34% of calls could yield daily savings of approximately $43,702, based on an average cost per call of $4.90.
Knowmax-powered self-service portals and chatbots deploy across web, mobile, and voice channels, integrating with EHR systems and CRMs to provide personalized responses. The platform has demonstrated a 60% query deflection rate, meaning six out of ten routine inquiries are resolved without agent involvement. This frees agents to focus on cases requiring clinical judgment, empathy, or multi-step problem-solving.
Sentiment-Aware Escalation and Contextual Handoff
Advanced AI agents detect frustration, urgency, or emotional distress in real time through tone and language cues. In healthcare, where patients may call about denied claims, delayed test results, or care access issues, recognizing emotion before it escalates into a formal complaint improves both FCR rates and patient satisfaction.
Where escalation is genuinely required, AI agents that transfer with full context (call summary, intent classification, patient history) ensure the receiving agent never asks the patient to repeat themselves. That context-rich handoff maintains the thread of the interaction and keeps the call resolvable within the same contact.
Types of AI Agents Driving FCR Improvement in Healthcare
Healthcare contact centers deploy four types of AI agents, each serving distinct functions:
1. Reactive agents respond to inbound queries in real time, answering questions or routing calls based on detected intent.
2. Proactive agents initiate outbound outreach for appointment reminders, care gap closures, medication adherence follow-ups, or open referral notifications.
3. Agent-assist (co-pilot) agents surface knowledge, next-best-action suggestions, and decision trees to human agents during live calls, enhancing resolution accuracy without replacing the agent.
4. Autonomous agents manage complete multi-step workflows end-to-end without human intervention—scheduling appointments, processing prescription refills, providing billing balances.
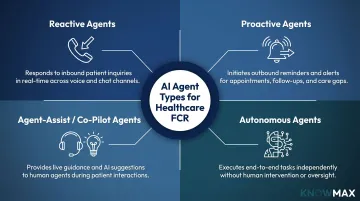
For FCR improvement specifically, the highest-impact deployments combine autonomous agents (for routine resolution) and agent-assist tools (for complex calls requiring human judgment with AI support). Most organizations start with one agent type and expand as they validate performance and mature their workflows. Whichever type you deploy, HIPAA compliance is non-negotiable.
HIPAA Compliance for AI Agents in Healthcare
AI agents handling protected health information must meet HIPAA requirements. The HHS HIPAA Security Rule mandates:
- Access control: Limits ePHI access to authorized personnel only through technical policies
- Audit controls: Records and examines all activity within systems that store or process ePHI
- Person or entity authentication: Verifies user identity before any system access is granted
- Transmission security: Protects ePHI from interception or unauthorized access during network transmission
- Encryption: Not mandated for a specific algorithm, but requires "reasonable and appropriate" measures based on a formal risk assessment
Healthcare organizations must obtain a signed Business Associate Agreement (BAA) from AI vendors before deployment. Knowmax maintains HIPAA certification with role-based access control, audit trails, encryption safeguards, and controlled content approval workflows, ensuring secure handling of patient data in contact center environments.
Key Metrics to Track When Measuring AI-Driven FCR Improvement
Measuring FCR accurately requires combining three data sources:
1. ACD/telephony records: Track whether the customer calls back for the same issue within a defined callback window. SQM Group notes that callback windows range from 1 to 30 days, with no universal standard. Shorter windows (7 days) capture true FCR more accurately, while longer windows risk counting unrelated contacts as failures.
2. Post-call patient surveys: Ask directly whether the issue was fully resolved. SQM Group considers this the gold standard for FCR measurement, as it reflects patient perception rather than system assumptions. Surveys conducted within one business day of the interaction yield the most reliable benchmarking data.
3. AI-generated conversation analytics: Score resolution based on transcript analysis and CRM update data. AI-powered automated QA can analyze 100% of customer calls, replacing manual sampling and identifying resolution patterns invisible in ACD data alone.
Supporting KPIs That Move Alongside FCR
Track these metrics to validate that FCR improvements are genuine, not statistical artifacts:
- Average Handle Time (AHT): Drops when agents surface accurate answers faster — without cutting corners on resolution
- Call abandon rate: Falls as smarter routing reduces queue pressure before patients give up
- Transfer rate: Declines when intent classification routes calls correctly on the first attempt
- Repeat call rate within 7 days: The clearest signal of genuine FCR improvement (or the lack of it)
- Patient satisfaction (CSAT/HCAHPS): Rises in step with FCR — when issues are truly resolved, patients notice
If AHT drops but repeat calls increase, FCR is not truly improving—agents may be rushing interactions without resolving the underlying issue.
Diagnosing these patterns requires connecting the right data sources. Platforms like Knowmax integrate with ACD and telephony systems (Genesys, Talkdesk) to correlate FCR and repeat contact data with knowledge base usage and agent guidance events. Conversation intelligence tools then analyze transcripts to surface recurring resolution failures, knowledge gaps, and misrouting patterns — turning metric monitoring into a continuous improvement cycle.

Frequently Asked Questions
Frequently Asked Questions
What are the 4 types of AI agents?
The four types are:
- Reactive agents — respond to inbound queries in real time
- Proactive agents — initiate outbound outreach
- Agent-assist (co-pilot) agents — surface knowledge and suggestions to human agents during live calls
- Autonomous agents — handle complete workflows end-to-end
Healthcare contact centers typically deploy a combination based on call type and complexity.
Are AI voice agents HIPAA compliant?
AI voice agents can be HIPAA compliant when built with appropriate safeguards: data encryption, access controls, audit trails, and a signed Business Associate Agreement (BAA). Healthcare organizations must verify these requirements are met before deployment.
What is a good FCR rate for healthcare contact centers?
The healthcare industry averages 71% FCR, with best-in-class human agent performance around 75% and world-class threshold at 80% or higher. AI-assisted contact centers typically achieve 80% to 85% FCR, though results vary based on call mix and baseline performance.
How do AI agents reduce repeat calls in healthcare?
AI agents reduce repeat calls through three mechanisms:
- Resolving routine inquiries completely on first contact
- Routing complex calls accurately so patients don't bounce between departments
- Delivering consistent knowledge to human agents so answers are right the first time
What types of healthcare calls benefit most from AI agent automation?
Appointment scheduling, prescription refill requests, billing balance inquiries, and referral status updates deliver the highest ROI from automation due to their high volume and relatively low complexity.
How does knowledge management support AI agent FCR performance?
Structured, up-to-date knowledge bases with guided resolution paths ensure both AI and human agents deliver correct answers consistently. Without accurate, well-organized knowledge backing them, even capable AI agents generate wrong answers — leading to callbacks and escalations that FCR improvements are meant to prevent.


