
Introduction
Healthcare contact centers handle an average of 2,000 calls daily, yet most centers are staffed to meet only 60% of peak demand. These calls span appointment scheduling, billing inquiries, insurance verification, and prior authorization status checks—the vast majority still handled manually by agents juggling multiple systems, long hold times, and repetitive questions.
The cost of this manual dependency shows up in every operational metric:
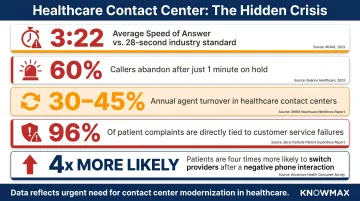
- Healthcare's average speed of answer is 3 minutes 22 seconds, seven times longer than the cross-industry standard of 28 seconds
- 60% of patients abandon calls after just one minute of waiting
- Agent turnover runs 30-45% annually, driven largely by burnout from repetitive work and inadequate support tools
- 96% of all patient complaints relate to customer service
- Patients are four times more likely to switch providers after a negative phone interaction
AI agents can automate much of this work, but healthcare contact centers operate under HIPAA, where the stakes of deploying AI incorrectly are severe. The average healthcare data breach now costs $9.77 million. Any disclosure of Protected Health Information (PHI) to an AI vendor without a signed Business Associate Agreement constitutes a notifiable breach.
None of this requires waiting. HIPAA-compliant AI agent use cases are deployable today, with documented ROI across both patient-facing automation and agent-assist workflows. This article covers what HIPAA compliance actually requires from AI systems, six use cases contact centers can implement immediately, and how to evaluate whether an AI platform is ready for a regulated healthcare environment.
TLDR
- Healthcare contact centers face dual pressure: call volumes rising faster than staffing capacity, and HIPAA obligations that most general-purpose AI tools cannot satisfy
- HIPAA-compliant AI requires more than encryption: BAAs, role-based access, audit trails, PHI minimization, and zero-retention policies are all mandatory
- Six high-impact use cases are ready now: scheduling, eligibility verification, prior auth tracking, billing self-service, agent-assist knowledge delivery, and proactive patient outreach
- The fastest ROI comes from pairing patient-facing automation with agent-assist AI that equips human agents with compliant, instant answers
What Makes an AI Agent HIPAA-Compliant for Contact Centers?
HIPAA compliance is not a badge—it is an architecture. For AI systems deployed in healthcare contact centers, compliance rests on three regulatory pillars: the Privacy Rule (45 CFR Part 164, Subpart E), which requires the "minimum necessary" use of PHI; the Security Rule (45 CFR Part 164, Subpart C), which mandates technical, physical, and administrative safeguards; and the Breach Notification Rule (45 CFR Part 164, Subpart D), which defines when and how breaches must be reported.
Generic AI tools—including most consumer-grade platforms—were not designed with these requirements in mind. Many retain user inputs to improve language models, a practice that becomes an immediate HIPAA violation when those inputs contain PHI. Any disclosure of PHI to a third-party AI tool without a signed Business Associate Agreement triggers breach notification obligations, even if the disclosure was unintentional.
Non-Negotiable Technical Requirements
Healthcare contact center AI must meet five core technical requirements:
- Business Associate Agreement (BAA): The vendor must sign a BAA and qualify as a Business Associate under 45 CFR 160.103, with subcontractor flow-down provisions
- End-to-end encryption: TLS 1.2+ for data in transit, AES-256 for data at rest
- Role-based access controls (RBAC): Access must be restricted by agent role, team, or content category, ensuring agents see only the PHI necessary for their function
- Immutable audit logs: Every interaction—queries, data access, escalations—must be logged in a tamper-proof format and exportable for compliance review
- Zero PHI retention or LLM training clauses: The vendor must contractually commit to not retaining PHI beyond the immediate transaction—not for model training, analytics, or any secondary use

Knowmax meets these enterprise healthcare compliance requirements with HIPAA, SOC 2, ISO 27001, and GDPR certifications, and integrates with leading CRM, telephony, IVR, and messaging platforms. Vendors missing even one of these requirements create compliance exposure that no feature set can offset—treat the checklist as a hard filter, not a preference.
Why Agentic AI Is Inherently Safer for HIPAA Environments
Agentic AI systems—those designed to operate on deterministic, policy-driven workflows—are fundamentally safer than open-ended generative AI for healthcare use cases. The core difference is architectural: generative AI produces text through statistical pattern-matching, which introduces hallucination risk. Agentic AI, by contrast, retrieves answers from a controlled knowledge base and routes actions within pre-defined boundaries.
That structural constraint matters enormously in HIPAA environments. Every output stays within the scope of verified, compliant content—there is no probabilistic inference, no improvised response.
For example, Knowmax's AI-powered search (Max AI) operates on policy-driven retrieval rather than open-ended generation. It surfaces answers from the organisation's approved knowledge base, medical literature, and protocols—not from speculative inference. Agents get accurate, auditable answers without the compliance risk that comes with generative output.
HIPAA-Compliant AI Agent Use Cases for Healthcare Contact Centers
The six use cases below represent the highest-volume, most rule-based workflows in healthcare contact centers — ideal starting points because each workflow is repetitive, structurally predictable, and carries low escalation risk with proper design.
Automated Appointment Scheduling and Rescheduling
AI voice and chat agents handle inbound and outbound appointment requests 24/7. They check provider availability, run a basic eligibility check, book slots, send confirmations, and route to a live agent only when urgent clinical flags are mentioned.
The gap between patient expectations and reality is wide: 89% of patients say 24/7 scheduling matters to them, yet only 11% of medical groups report that a majority of patients self-schedule. Patients average 3.5 calls per scheduling need — a volume problem AI can eliminate.
HIPAA design requirements:
- Collect only minimum necessary PHI: name, date of birth, appointment type
- Block prompts for clinical details not required for scheduling
- Verify caller identity before surfacing any appointment history
Ineffective scheduling contributes to over $150 billion in lost revenue annually for the healthcare industry. Automating this workflow reduces call volume, eliminates hold times, and redirects agents to calls that actually need them.
Insurance Eligibility Verification and Benefits Queries
Patients calling to confirm coverage, co-pays, deductibles, or in-network status can be served by AI agents that authenticate the caller, query eligibility data from payer systems or clearinghouses, and return accurate benefit summaries — without placing humans on hold with payers.
HIPAA design requirements:
- Verify caller identity before surfacing any PHI
- Deliver benefit details in-session without retaining them in unsecured logs
- Log every query with a complete audit trail
The 2023 CAQH Index puts manual eligibility verification at $12.56 per transaction versus $2.22 electronically — a $10.34 savings per check, representing a $9.3 billion national opportunity. Few automation investments in healthcare have clearer math.
Prior Authorization Status Tracking and Initiation
AI agents handle inbound calls from patients or provider offices checking PA status, provide real-time updates by querying payer portals or internal RCM systems, and initiate standard authorization requests by collecting required clinical criteria and routing the complete package to the appropriate team.
HIPAA design requirements: Prior authorization workflows involve diagnosis codes, medication names, and clinical history — all PHI. AI agents must apply strict data minimization rules, and every query and action requires a complete audit trail.
Practices process 39 prior authorization requests per physician per week, burning 13 hours of staff time. Forty percent of physicians now employ staff dedicated exclusively to PA. Automating status checks and document gathering converts that fixed overhead into recaptured capacity.

Billing and Claims Inquiry Self-Service
AI agents handle the highest-volume billing queries — balance inquiries, explanation of benefits questions, payment plan eligibility, and claim status checks — by authenticating the caller, pulling data from billing systems, and delivering plain-language answers. For complex disputes, the agent collects context and routes to a billing specialist with full context attached.
HIPAA design requirements:
- Never surface another patient's data — enforce strict identity verification before accessing any financial or claims record
- Log every interaction and tie it to the authenticated user
Billing and payments drive 52% of healthcare contact center call volume — the single largest inbound category. 37% of patients report missing a medical bill because the process was too confusing. Self-service billing AI addresses both problems: fewer calls, fewer missed payments.
AI-Guided Agent Assist for Complex Healthcare Queries
Not all calls can or should be fully automated. For complex queries — multi-step clinical eligibility questions, complaints, sensitive situations — human agents still take the call. But AI agent-assist tools can surface the right answer instantly, guiding the agent through decision trees, compliance-aware scripts, and knowledge base content in real time.
This reduces average handle time, eliminates agent error on sensitive healthcare topics, and ensures every agent gives the same compliant answer regardless of experience level.
Knowmax's AI-powered search, guided decision trees, and omnichannel knowledge delivery give agents accurate, up-to-date answers instantly — no searching across siloed systems, no relying on memory. Because Knowmax is HIPAA-certified, the knowledge layer itself meets the compliance requirements of the contact center environment. Consistent, guided delivery also reduces compliance exposure from agent improvisation.
Healthcare contact center first call resolution averages just 52% — well below the industry standard of 70–79%. Agent-assist knowledge tools are the primary lever for closing that gap without full automation.
Proactive Outreach: Appointment Reminders, Care Gap Alerts, and Follow-Ups
Healthcare contact centers are not only inbound. Outbound AI agents can send HIPAA-compliant appointment reminders, medication adherence nudges, post-discharge follow-up calls, and care gap notifications — through the patient's preferred channel (SMS, voice, email) with proper opt-in management and PHI minimization.
HIPAA design requirements:
- Apply the minimum necessary standard in every message (e.g., "You have an appointment on Tuesday," not diagnosis details)
- Confirm patient consent before any digital outreach
- Log all message delivery
The average outpatient no-show rate sits at 23% across specialties, costing U.S. providers an estimated $150 billion per year. Automated reminder outreach cuts no-shows by up to 38% — a direct, measurable return on a workflow that requires no clinical judgment to deploy.
The Two Sides of Healthcare Contact Center AI: Patient-Facing vs. Agent-Assist
Most discussions of healthcare AI conflate two distinct deployment models: patient-facing AI (chatbots, voice agents, self-service portals) and agent-assist AI (tools that work behind the scenes to make human agents faster, more accurate, and more compliant). Both are necessary, and both must be HIPAA-compliant—but they solve different problems and carry different risk profiles.
Risk Profile Difference
Patient-facing AI carries higher stakes for errors because there is no human check before the patient receives information. Agent-assist AI has a human in the loop, making it a safer starting point for organizations new to healthcare AI deployment.
For most contact centers, the lower-risk path is to deploy agent-assist AI first—where errors get caught before they reach the patient—then expand to patient-facing automation for high-volume, low-stakes workflows like appointment reminders and billing FAQs.
What a Mature Model Looks Like
In a mature deployment, each layer handles what it does best:
- Patient self-service handles routine scheduling, billing FAQs, and status checks
- Agent-assist tools equip human agents for complex, sensitive, or escalated interactions
- Every layer maintains a consistent knowledge foundation and audit trail
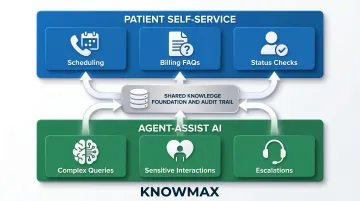
The result is fewer escalations, faster resolutions, and a compliance trail that holds up to audit — without compromising the patient experience at any touchpoint.
Evaluating HIPAA-Ready AI Platforms: What Healthcare Contact Centers Should Demand
Healthcare contact centers evaluating AI vendors should apply a strict compliance and integration checklist:
Compliance Requirements:
- Will the vendor sign a BAA?
- Does the system support role-based access controls that match the contact center's agent permission levels?
- Are audit logs immutable and exportable for compliance review?
- Does the platform have published certifications (SOC 2 Type II, ISO 27001, HIPAA) rather than self-attestation?
- Does the LLM or AI layer have a zero-retention or no-training clause for PHI?
Integration Requirements:
Compliance doesn't stop at the platform boundary. Ask vendors:
- Does the platform integrate with EHRs, payer portals, billing systems, and CRM tools without exposing PHI at handoff points?
- How is PHI handled during API calls to external systems?
- Do subcontractors also operate under BAAs, or only the primary vendor?
Knowmax holds HIPAA, SOC 2, ISO 27001, and GDPR certifications and integrates with CRM, telephony, IVR, and messaging platforms — including Salesforce, Zendesk, Genesys, Talkdesk, and Freshdesk. For healthcare contact centers, that combination of verified compliance and deep integration support means agents get AI-assisted knowledge delivery without creating new PHI exposure points.
Frequently Asked Questions
Frequently Asked Questions
What does HIPAA compliance mean for AI tools used in a healthcare contact center?
HIPAA compliance for AI requires a signed Business Associate Agreement, technical safeguards (encryption, access controls, audit logs), PHI minimization, and zero-retention policies—not just a general privacy policy or self-attestation claim.
Can AI agents in a healthcare contact center access or share patient health information?
Yes, but only under strict conditions:
- The caller must be authenticated before any PHI is accessed
- Only the minimum necessary PHI should be retrieved per interaction
- Every interaction must be logged in an auditable trail
- The AI vendor must be covered under a signed BAA as a Business Associate
What is the difference between a HIPAA-compliant AI agent and a regular chatbot?
A standard chatbot answers scripted questions and may retain inputs for model training—a direct HIPAA violation. A compliant AI agent operates on deterministic workflows, applies PHI safeguards, enforces access controls, and logs every action in an auditable trail.
How do AI agents improve first call resolution in healthcare contact centers?
AI agents improve FCR by surfacing accurate, real-time information (eligibility, claim status, scheduling availability) instantly—eliminating holds, callbacks, and agent knowledge gaps that cause repeat contacts.
Do healthcare contact centers need a Business Associate Agreement with every AI vendor they use?
Yes. Any vendor whose platform creates, receives, maintains, or transmits PHI on behalf of a covered entity is a Business Associate under HIPAA and must sign a BAA before deployment—including AI platform providers, cloud hosts, and subcontractors.
Should healthcare contact centers start with patient-facing or agent-assist AI deployments?
Start with agent-assist AI. The human-in-the-loop model limits risk while building internal confidence—then expand to patient-facing automation for high-volume, well-defined workflows like appointment reminders and billing FAQs.


