
Introduction
Insurance customers expect fast, accurate resolutions, but traditional workflows regularly fail to deliver. Carriers spend $7–$15 per document with up to 25 documents per claim, creating administrative costs of $375 before a coverage decision is made. Average property claim cycles still run approximately 30 days, and during catastrophe events, manual error rates spike from 1–4% to as high as 40%.
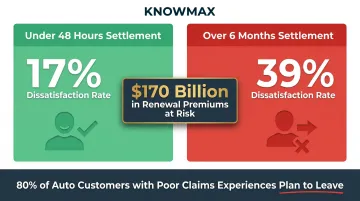
The cost goes beyond processing time. Approximately 70% of insurance customer churn stems from poor claims experiences, putting $170 billion in renewal premiums at risk over five years. Customers who wait over 6 months for settlement show 39% dissatisfaction rates compared to just 17% when claims settle under 48 hours.
Both problems — cost overruns and eroding customer loyalty — trace back to the same root cause: slow, manual workflows. AI workflow automation is now compressing these timelines across multiple insurance functions: claims intake, underwriting, fraud detection, policy servicing, and renewals. This article covers where AI delivers the biggest speed gains, which technologies drive them, and what outcomes insurers are actually documenting.
TLDR
- AI cuts claims processing time by 50-80%, with leaders like Allianz achieving reductions from 4 days to hours
- NLP, computer vision, and intelligent document processing automate intake, triage, and document extraction end-to-end
- Straight-through processing handles eligible claims with zero human touchpoints
- Fraud detection at intake protects revenue while accelerating legitimate claims
- Structured knowledge management ensures agents and AI alike resolve claims accurately — not just quickly
Why Traditional Insurance Processing Creates Costly Bottlenecks
Manual insurance workflows share three persistent problems:
- Disconnected systems that require repeated data entry across platforms
- Multi-layer approvals slowing down routine transactions
- Error rates that trigger costly rework cycles
Underwriters spend up to 40% of their time on administrative tasks rather than core decision-making — contributing to an estimated $160 billion industry-wide efficiency loss over five years.
Claims professionals reviewing medical records for Medicare Set-Aside cases spend 15–20 hours per claim, with 30–40% of that time consumed by manual document organisation alone.
Impact on Customers and Retention
These structural inefficiencies flow directly to the customer experience:
- 58% of insurers admit slow claim payouts drive customer churn
- Dissatisfaction correlates directly with settlement speed: 17% dissatisfied under 48 hours vs. 39% over 6 months
- 80% of auto insurance customers with poor claims experiences plan to leave their provider
Volume Spikes Expose Scalability Limits
These same workflow constraints peak during catastrophe events. Hurricane claims generate 2–3x normal volume within days, and manual error rates simultaneously spike from 1–4% under normal conditions to 18–40% under time pressure. Manual workflows cannot absorb these surges, creating immediate backlogs that compound customer dissatisfaction.
The AI Technologies Making Insurance Automation Possible
Natural Language Processing (NLP)
NLP enables AI to extract structured data from unstructured insurance documents—emails, medical records, police reports, handwritten claim forms—replacing hours of manual review. One carrier uses AI to generate approximately 50,000 claims-related communications daily to improve clarity and empathy.
For Medicare Set-Aside claims, where professionals manually review 300-500 pages per case, 30-40% of review time is spent just organizing and navigating documents. NLP-powered systems handle digitization and sequencing automatically, letting adjusters focus on analysis rather than administration.
Computer Vision
Computer vision assesses property and vehicle damage from submitted photos and videos, generating repair estimates automatically and reducing physical inspection requirements in routine cases.
GEICO deployed Tractable's AI Review, which assesses auto damage estimates within seconds compared to the traditional 30-minute review. The system reviews 50% of claims without human involvement and cuts an average of 8 days from cycle times.
Drones and satellite imagery enable rapid assessment during natural disasters, allowing carriers to triage claims based on actual damage severity before adjusters arrive on-site.
Machine Learning and Predictive Triage
ML algorithms analyze historical claims data to automatically route submissions by complexity: simple claims proceed directly to automated settlement, while complex cases go to experienced adjusters.
Real-world results show what accurate routing can deliver:
- Aviva (UK) deployed 80+ AI models in claims, achieving a 30% improvement in routing accuracy
- Compensa Poland implemented AI-based FNOL, segmentation, and routing, achieving a 10% improvement in claims accuracy
Predictive analytics extend this further — flagging denial risks early so teams can reach out to policyholders before disputes escalate.
Intelligent Document Processing (IDP)
IDP combines OCR, NLP, and ML to ingest, validate, and update claims data across systems in real time. Where manual data entry carries a 1–4% error rate under normal conditions, IDP reaches 99.5–99.9% accuracy even on semi-structured documents like varied invoices and work orders.
In one deployment, error rates dropped from 4.2% to 0.6% — and the document handling step that typically caused the longest delays was eliminated entirely.
Agentic AI: Multiple Agents Collaborating
Allianz's Project Nemo is the first integrated agentic AI solution deployed in production. Launched in Australia in July 2025, it targets low-complexity, high-volume claims—specifically food spoilage claims under 500 AUD triggered by natural catastrophe events.
Seven specialized AI agents collaborate:
- Planner Agent: orchestrates workflow
- Cyber Agent: enforces data security
- Coverage Agent: verifies policy coverage
- Weather Agent: cross-references meteorological data
- Fraud Agent: applies ML pattern recognition
- Payout Agent: calculates settlement amounts
- Audit Agent: generates decision summary for human review
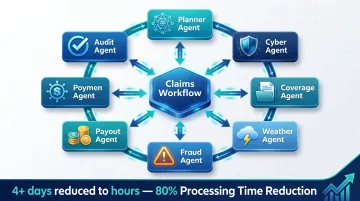
Processing time reduction: 80% reduction in claim processing and settlement time. The AI workflow completes in under 5 minutes; total time reduced from 4+ days to hours. The system was deployed from scope to live in under 100 days.
Human review remains mandatory—payout decisions are never fully automated. A claims professional must approve the Audit Agent's summary before final payment authorization.
AI Workflow Automation Across the Insurance Value Chain
Speed gains are occurring simultaneously across multiple functions—this "across the board" scope distinguishes modern AI adoption from earlier point-solution automation.
Automated FNOL and Claims Intake
Chatbots and virtual agents now handle First Notice of Loss end-to-end: guiding policyholders through reporting, collecting documentation, and logging the claim without routing through a call center.
The numbers show how far this has come:
- Lemonade's chatbots handle 96% of FNOL without human intervention
- 55% of all claims resolve fully automated, in seconds rather than weeks
- Liberate Voice AI completed FNOL calls in 7 minutes 10 seconds vs. 12 minutes for traditional intake
This compresses initial intake from 15–30 minutes to seconds and frees agents for escalations.
Straight-Through Processing for Simple Claims
For low-complexity claims, AI systems automatically verify policy details, validate the claim, approve the payout, and trigger settlement with zero human touchpoints.
Up to 95% of personal lines policies may undergo straight-through processing with no underwriter involvement. One midsize P&C insurer expects to more than double STP rates within 1–2 years, cutting issuance and binding time by 50%.
Fraud Detection at Intake
Speed gains from STP only hold if fraud is caught before—not after—payout. AI fraud detection now happens at the verification stage, not post-processing. The stakes are significant: an estimated 10% of all P&C claims are fraudulent, costing $122 billion annually, yet current soft fraud detection rates sit at only 20–40%.
AI-driven multimodal detection applies anomaly detection across thousands of variables before any payout occurs — a shift that could save insurers $80–$160 billion by 2032.
Policy Servicing and Renewals
AI automates endorsements, certificate issuance, and renewal reminders—tasks that are repetitive, high-volume, and low-complexity but consume significant agent time.
Agencies implementing automated renewal workflows report 98.4% retention rates. That freed capacity shifts agents toward complex policy changes and cross-sell conversations where human judgment actually adds value.
Measurable Outcomes: What Insurers Are Seeing After Automation
The data coming out of early AI deployments in insurance isn't incremental — it's a category shift. Here's what insurers are reporting across processing speed, accuracy, cost, and customer experience.
Processing Time Reductions
| Insurer/Deployment | Time Reduction | Detail |
|---|---|---|
| Allianz Project Nemo | 80% reduction | 4+ days to hours for NatCat food spoilage claims |
| Aviva (80+ AI models) | 23 days reduced | Liability assessment time for complex cases |
| GEICO/Tractable | 8-day cycle reduction | Claims cycle shortened by 8 days; damage photo review cut from 30 min to seconds |
| Lemonade | Seconds vs. weeks | 55% of claims fully automated end-to-end |

Error Rate Improvements
Manual data entry error rates of 1-4% under normal conditions spike to 18-40% during catastrophe events. AI-assisted systems achieve 99.5-99.9% accuracy, maintaining error rates below 0.5% even during volume surges — precisely when manual accuracy degrades most.
Cost Savings
- Aviva saved over £60 million in motor claims
- Compensa Poland achieved 73% increase in cost efficiency
- Customer onboarding costs dropped 20-40% through automated document verification workflows
- AI fraud detection models show 20-40% savings potential by flagging anomalies that manual review routinely misses
Customer Experience Impact
Aviva reported a 65% reduction in customer complaints after deploying 80+ AI models in claims. An insurer that moved 80% of transactions online saw customer referral likelihood rise by 36 percentage points.
That referral lift makes sense when you consider what's driving call volume: 40% of inbound contacts are basic claims status checks, a workload that self-service automation absorbs without adding headcount.
How Knowledge Management Supercharges AI Workflow Automation
The Resolution Gap Automation Alone Doesn't Close
When AI systems route complex claims to agents, or when customers escalate beyond automated paths, agents need instant access to accurate, structured knowledge to avoid delays, errors, and repeated callbacks.
Claims calls have the lowest First Call Resolution (FCR) rate of any insurance call type: just 61% compared to the industry average of 73-75% and world-class standard of 80%+. Every 1% improvement in FCR yields $286,000 in annual savings for a midsize call center.
Nearly 49% of non-FCR calls fail due to organizational errors—information access issues, process complexity, and knowledge gaps—rather than agent mistakes. A knowledge management gap is one of the most common reasons AI-assisted workflows still result in high Average Handling Time (AHT).
How AI-Powered Knowledge Management Closes the Gap
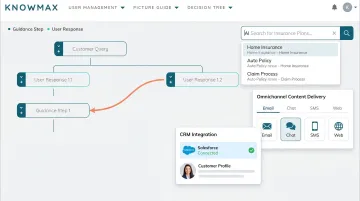
Platforms like Knowmax address this directly through:
- Guided decision trees that walk agents through complex claim or policy scenarios step by step, enforcing compliance with regulatory requirements and reducing errors at each decision point
- Intent-based AI search — unlike keyword systems requiring exact matches, NLP-driven search surfaces contextually relevant content (policy details, underwriting guidelines, claims procedures) even when agents don't use precise phrasing
- Omnichannel delivery that ensures the same accurate information is available on calls, chat, or self-service portals, with CRM integrations for Salesforce, Zendesk, and Genesys so agents never toggle between screens
- Automatic content versioning with authorization workflows, so agents always act on current policy rules rather than outdated procedures
These capabilities connect directly to resolution outcomes—and the numbers are measurable.
Measurable Impact on Resolution Metrics
When agents have instant, accurate knowledge at their fingertips:
- FCR improves — each percentage point gained translates to six-figure annual savings for a midsize contact center
- AHT drops — documented cases show 15-21% reductions in handling time and 46% decreases in overall call volume
- Escalations decrease, preserving the productivity gains from front-end AI automation rather than losing them in the resolution layer
The average AHT for financial services and insurance contact centers is currently 4 minutes 45 seconds. When agents cannot find information quickly, AHT increases—negating the speed benefits of automated intake and triage.
Frequently Asked Questions
What is the role of AI in automating insurance claims processing?
AI automates data extraction, validation, fraud detection, and payout decisions across the claims lifecycle. By eliminating manual touchpoints, AI compresses processing from days to hours or minutes.
What are the benefits of AI workflow automation?
Core benefits include 50-80% faster processing times, 20-40% lower operational costs, sub-0.5% error rates, multimodal fraud detection, and improved customer satisfaction through faster claim resolution.
Which insurance workflows benefit most from AI automation?
High-impact areas include FNOL intake, claims validation and settlement, fraud detection at verification stage, policy renewals, endorsements, and certificate issuance. Any high-volume, low-complexity workflow with structured decision logic is a strong candidate.
What is straight-through processing in insurance?
Straight-through processing (STP) refers to low-complexity claims being automatically verified, approved, and settled by AI without any human intervention. Up to 95% of personal lines policies may qualify for STP, enabling near-instant resolution.
How long does it typically take to implement AI workflow automation in insurance?
Timelines vary by scope, but phased approaches starting with high-volume, low-complexity workflows can deliver initial results within weeks. Allianz's Project Nemo, for instance, went from scoping to live deployment in under 100 days.


