
Introduction
Insurance CX leaders face a frustrating paradox. AI budgets are climbing, adoption rates are surging across the industry, yet many contact centers report CSAT scores and First Call Resolution (FCR) rates that have barely budged. The reality is that not all AI investments deliver equal impact.
That gap shows up clearly in the numbers: 88% of contact centers now use some form of AI, yet only 14% of customer issues actually resolve through self-service channels. Deployment and measurable outcomes are not the same thing — and the distance between them is where most AI investments quietly stall.
What follows is a practitioner's guide to the specific AI applications demonstrably improving FCR, Average Handle Time (AHT), and CSAT in insurance support — and why placement in the workflow matters more than the tool itself.
TLDR
- AI impact in insurance CX concentrates in specific use cases: agent-assist tools, intelligent claims intake, and AI-powered knowledge access
- Agent-side AI delivers faster, more measurable ROI than customer-facing chatbots in insurance environments
- Fragmented knowledge is the top reason AI tools underperform — responses break down on complex policy queries
- High-performing teams use AI to guide agents, not just deflect customers, and measure FCR and AHT — not just containment rates
The CX Pressure Points Unique to Insurance Support Teams
Why Insurance Contact Centers Face Structural Complexity
Insurance operates in a structurally harder CX environment than most industries. Interactions carry high emotional stakes — especially claims filed during loss events. Policy language remains dense and technical. Regulatory compliance requirements are strict. Query complexity varies wildly, from simple billing updates to multi-step coverage disputes.
Insurance contact centers average 4.01 minutes in AHT, significantly above telecommunications (2.56 minutes) and eCommerce (3.41 minutes). When wrap-up time is included, the industry average climbs to 697 seconds (11.6 minutes) — an 18% year-over-year increase.
That's not inefficiency — it's the nature of the work. Each call requires multi-system lookups, regulatory validation, and careful explanation of technical policy terms to customers who are often already stressed.
The Agent Experience Problem
Insurance support agents juggle dozens of policy types, pull information from scattered knowledge sources, and face high cognitive load on every interaction. 76% of insurance employees spend more than 30% of their workday searching for correct information, while 37% of frontline agents have no knowledge base at all.
Agent turnover compounds the problem. Contact center attrition hovers around 34% annually, with both turnover and work-from-home rates roughly double pre-COVID levels.
Customer Expectations vs. Reality
Policyholders want fast, accurate answers with empathetic handling. The data shows how far most insurers fall short:
- 59% of customers cite resolution time as their biggest complaint with call centers
- 80% of auto insurance customers with poor claims experiences have left or plan to leave their insurer
- 64% of consumers would switch insurers for a better digital experience
- 22% have avoided filing claims altogether because the process felt too frustrating
What "Moving the Needle" Actually Means
For insurance CX leaders, measurable success means improvement in four core metrics:
- First Call Resolution (FCR): Industry average sits at 73-75%, but claims-specific FCR drops to just 61%
- Average Handle Time (AHT): 697 seconds industry-wide, with variation across query types
- Customer Satisfaction (CSAT): Health insurance averages 76/100, life insurance 78/100
- Escalation Rate: Typical Tier-1 escalation ranges from 5-15%

Many insurers have AI tools deployed but haven't moved any of these numbers. The gap isn't about adoption — it's about where the AI is applied. The sections below break down which tools are actually shifting these metrics, and why.
AI Tools That Are Actually Moving CX Metrics
Impact in insurance CX concentrates in four AI application types: conversational AI for claims intake, AI-assisted agent guidance, intelligent routing and triage, and AI-powered self-service for routine policy queries. Each addresses different workflow friction points.
Conversational AI for Claims Intake (FNOL)
AI-powered first notice of loss intake — via voice or chat — reduces handling time for the highest-stress interaction in insurance CX. The system captures required claim details, verifies policy information, and initiates the claims file automatically, reducing burden on live agents.
Current adoption: 38% of customers used digital tools to report FNOL, meaning the majority still involve live agents. However, insurers deploying FNOL automation report dramatic improvements. One carrier reduced claim processing time from 45 minutes to 10 minutes through automation.
The retention stakes are substantial. Beyond the 80% customer churn tied to poor claims experience, claim handling delays accounted for 22.8% of total closed insurance complaints in 2023 — surpassing denials and unsatisfactory settlements combined.
AI-Assisted Agent Guidance During Live Interactions
This category most directly moves FCR and AHT in insurance contact centers. Real-time agent assist tools surface relevant knowledge, suggest next steps, and flag compliance considerations during live calls — reducing agent hesitation, errors, and escalations.
A controlled A/B test with 100 agents handling 40,000 interactions showed agentic AI reduced AHT by 38% — from 4 minutes 43 seconds to 2 minutes 55 seconds. The same deployment achieved a 33% uplift in lead-to-enquiry conversion.
In insurance, policy complexity makes it unrealistic to rely on agent memory alone. When agents navigate dozens of product variations and regulatory requirements, real-time knowledge retrieval is what separates accurate first-contact resolution from costly escalation.
Platforms like Knowmax embed decision trees and guided workflows directly into agent desktops, providing step-by-step assistance during complex queries — ensuring compliance while accelerating resolution. That matters when 76% of employees spend over 30% of their day searching for information.
Intelligent Routing and Triage
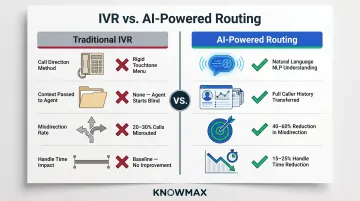
AI-based routing uses natural language processing to understand customer intent from initial contact, reducing misdirected calls and repeat contacts. Traditional IVR systems misdirect 20-30% of calls, forcing customers to repeat information and agents to handle queries outside their expertise.
AI-powered intent routing reduces transfer rates by 40-60% and handle time by 15-25%. When a customer calling about a claim routes directly to a claims specialist instead of a general queue, FCR improves immediately — especially important since escalated calls carry 2-4x the AHT of first-contact resolutions.
The key distinction: basic IVR relies on touchtone menu selections and passes zero context to the receiving agent. AI routing pulls caller history, understands natural language intent, and matches to the most qualified available agent — all before the conversation begins.
Automated Self-Service for Routine Policy Queries
Chatbots and virtual assistants have had mixed results in insurance. The difference between success and frustration comes down to realistic scoping.
Self-service AI works for:
- Payment status checks
- Basic coverage questions
- Document requests
- Renewal reminders
- Policy ID card access
Self-service AI creates frustration for:
- Coverage disputes
- Complex claim questions
- Emotionally sensitive situations
- Multi-step policy changes
Insurance chatbots resolved 34.7% of all chats in the sector — trailing the banking sector by a wide margin. Customer expectations are nuanced: 69% prefer self-service when it works successfully, but 72% won't reuse a chatbot after a single negative experience.
Self-service AI earns its place on high-volume, low-complexity queries where accuracy risk is minimal. Anything complex or emotionally charged still needs a human agent.
The Knowledge Layer: Why Most AI Deployments Underperform Without It
The majority of AI failures in insurance CX trace back to a knowledge problem, not a technology problem. AI tools — whether chatbots, agent assist, or voice bots — are only as accurate and useful as the knowledge they draw from. When that knowledge is outdated, siloed in PDFs, or inconsistent across channels, AI responses will be wrong or contradictory.
What This Looks Like in Practice
An agent-assist tool surfaces different answers depending on which knowledge base it pulls from. A chatbot gives a policyholder incorrect coverage information because the underlying content was last updated two product cycles ago. A new agent can't trust the AI suggestion because they've seen it be wrong before.
These aren't edge cases. When 37% of frontline agents have no knowledge base at all, and most others navigate fragmented sources, AI built on that foundation inherits the dysfunction.
What AI-Ready Knowledge Management Looks Like
A proper knowledge layer needs more than a searchable database. It requires deliberate architecture across five dimensions:
- Centralizes content into one repository so agents and self-service channels never pull from conflicting sources
- Structures information as decision trees, visual guides, and FAQs — formats AI can actually parse and surface accurately
- Syncs updates in real time across agent desktops, self-service portals, and chatbots simultaneously
- Delivers role-appropriate content — claims specialists see different articles than billing agents
- Routes regulatory changes directly into knowledge workflows, so compliance gaps don't accumulate
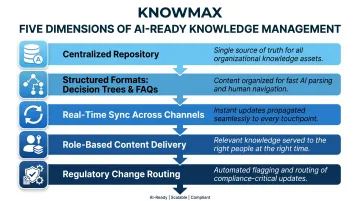
Platforms built for this purpose — Knowmax among them — go further by applying intent-based search that returns relevant results even when agents phrase queries inconsistently, and by delivering the same verified content whether the request comes through an agent desktop, a chatbot, or a customer-facing portal.
The Metric Connection
Teams that invest in knowledge management as the foundation of their AI stack see higher FCR and lower AHT because agents get the right answer on the first attempt, and self-service tools stop generating escalations from wrong answers. Modern knowledge platforms can reduce search time by 65% and call volume by up to 40%.
Agent-Assist vs. Customer-Facing AI: What Actually Works in Insurance
Most AI investment discussions focus on customer-facing AI — chatbots and virtual agents — because it promises deflection and cost savings. The economic case is clear: median cost per contact is $1.84 for self-service versus $13.50 for agent-assisted interactions.
But in insurance, where interactions are complex and high-stakes, agent-assist AI often delivers faster and more durable CX improvement.
Why Agent-Assist Delivers Faster ROI
Customer-facing AI works best for high-volume, low-complexity queries. In insurance, a disproportionate share of contact center volume involves nuance — coverage interpretation, claims disputes, underwriting questions — where fully automated responses increase escalation risk.
Agent-assist AI improves the quality of human conversations rather than replacing them. Key capabilities include:
- Cuts information retrieval time from 5–9 seconds per query to under 0.5 seconds
- Ensures compliance through guided workflows at the point of conversation
- Pulls in relevant customer history to support more personalized responses
The 38% AHT reduction documented in controlled testing came from agent-assist deployment, not customer-facing bots. Similar research involving 5,000 agents showed generative AI increased issues resolved per hour by 14–15%.
A Practical Decision Framework
Map query types by complexity and emotional sensitivity:
| Query Type | Complexity | Emotional Sensitivity | AI Approach |
|---|---|---|---|
| Payment status | Low | Low | Self-service AI |
| Document request | Low | Low | Self-service AI |
| Coverage question (basic) | Medium | Low | Self-service with escalation path |
| Claims status update | Medium | Medium | Agent-assist (human-led) |
| Coverage dispute | High | Medium | Agent-assist (human-led) |
| Active claim during loss | High | High | Agent-assist (human-led) |
Most insurance contact centers need both approaches, but the ratio matters. Prioritize agent-assist for the interactions that define customer perception of your brand: claims, disputes, and complex policy changes. Self-service works best for transactional queries where automation genuinely improves customer convenience.
How to Measure Whether Your Insurance AI Investment Is Working
Focus on Resolution, Not Deflection
The most common measurement mistake: tracking containment rate (how many queries the chatbot "handled") as the primary success metric. Containment measures deflection, not resolution. A customer who abandons in frustration counts as "contained" but not "resolved."
Basic bots achieve 20-40% containment while leaders reach 80-90%, but the key metric is recontact rate within 24-72 hours. If customers return with the same issue, the AI deflected rather than resolved.
Track the Right Metrics
Primary metrics for insurance AI success:
- FCR: Insurance benchmark 73-75% overall, 61% for claims; world-class is 80%+
- AHT: Industry average 697 seconds; improvement of 15-25% indicates effective AI deployment
- Post-interaction CSAT: Health insurance benchmark 76/100, life insurance 78/100
- Escalation rate: Typical Tier-1 range 5-15%; below 10% is good, below 5% is world-class

Secondary metrics:
- Containment accuracy (not just rate)
- Recontact rate within 24-72 hours
- Agent utilization of AI suggestions
- Knowledge base search success rate
Once you know what to track, the next step is structuring measurement so AI's contribution is clearly visible.
Before/After Measurement Approach
Attributing impact to AI tools requires baseline metrics before deployment and consistent measurement windows post-deployment. Segment results by query type — improvements in claims intake AHT shouldn't be diluted by unchanged performance in policy endorsements.
Each 1% improvement in FCR yields $286,000 in annual savings for a typical midsize call center and increases interactional NPS by 1.4 points.
The Feedback Loop
AI tools that sustain improvement are continuously refined. Teams that see lasting gains review escalation data, identify where AI suggestions were wrong or ignored, and use that to update their knowledge base and retrain models.
This is why knowledge management and AI are not separate investments — they compound each other.
Manual QA typically samples only 2-5% of calls. AI-powered QA scores 100% of interactions, surfacing failure patterns that traditional measurement simply cannot detect.
Frequently Asked Questions
How are insurance companies using AI to improve customer experience?
Insurance companies deploy AI across four primary use cases: automating routine inquiries via chatbots, using AI-assisted agent tools to improve resolution accuracy during live calls, automating claims intake (FNOL), and personalising interactions through predictive analytics. Each use case targets a different friction point — faster response, higher accuracy, or better compliance — rather than a single blanket improvement.
Will AI replace insurance customer service?
AI is augmenting rather than replacing human agents in insurance. Given the complexity and emotional weight of insurance interactions — especially claims during loss events — AI handles repetitive, structured tasks while human agents focus on complex coverage decisions, disputes, and empathetic claims handling where judgment and reassurance matter most.
What metrics should insurance teams track to measure AI impact on CX?
Track First Call Resolution (FCR), Average Handle Time (AHT), post-interaction CSAT, escalation rate, and chatbot containment accuracy as the most meaningful indicators. Containment rate alone is insufficient and can be misleading — pair it with recontact rate within 24-72 hours to measure true resolution, not just deflection.
Which AI tools help insurance agents resolve queries faster during live calls?
Real-time agent assist tools, AI-powered knowledge search, and guided decision trees surface the right information during live interactions — reducing hold time and cutting unnecessary escalations. They integrate directly into agent desktops, delivering compliance-aware recommendations based on customer history and policy details within a single interface.
How does knowledge management support AI performance in insurance contact centers?
AI tools are only as accurate as the knowledge they access. A centralised, structured knowledge base with decision-tree logic ensures consistent, correct answers across every channel — without it, AI inherits fragmented or outdated information, producing wrong answers that damage CSAT and drive escalations up.


