
Introduction
Healthcare teams face an overwhelming knowledge challenge. Clinicians, administrators, and contact center agents navigate fragmented information scattered across EHRs, departmental wikis, email threads, and printed SOPs. Medical knowledge now doubles approximately every 73 days, and manual methods can't keep pace. Acting on outdated protocols or incorrect information doesn't just slow workflows — it creates direct patient safety risks.
Traditional knowledge management systems were built for slower-moving information environments. They rely on manual updates, keyword search, and static documents that quietly go stale — a structural mismatch for healthcare, where clinical guidelines, drug interactions, insurance policies, and regulatory requirements shift constantly.
The result shows up at the point of care. When a nurse searches for "post-op wound care for diabetic patients" and gets a list of generic, unranked documents instead of a direct answer, time is lost and errors become more likely.
This article examines the AI capabilities transforming healthcare knowledge management right now — deployable tools solving real problems. You'll see how semantic search, automated content maintenance, guided workflows, and proactive knowledge delivery help clinical and support teams keep pace with healthcare's information velocity.
TLDR
- Traditional healthcare KM systems create dangerous information gaps through manual updates and keyword-only search
- AI enables semantic search and role-based knowledge delivery at the speed healthcare operations demand
- Clinical staff, contact center agents, and administrative teams all benefit from AI-guided access to verified protocols
- Measurable outcomes include fewer medical errors, faster query resolution, and reduced training time
- Success depends on HIPAA-compliant platforms with built-in clinical validation and change management support
Why Traditional Healthcare Knowledge Management Falls Short
Healthcare organizations store critical knowledge across EHRs, shared drives, departmental wikis, email threads, and printed SOPs. This fragmentation makes consistent access nearly impossible — approximately 80% of medical data remains unstructured and untapped after creation, locked in formats that traditional search tools can't surface effectively.
The daily toll is tangible. A junior doctor on call may spend 59.5% of their time reviewing notes and 13% searching for information — roughly 30 minutes of a 4-hour shift — citing search as one of their biggest frustrations.
Fragmentation isn't the only failure. Knowledge decay works alongside it: Clinical protocols, drug guidelines, and insurance policies change frequently, but static documents update silently without mechanisms to notify staff or flag stale content. Approximately half of clinical guidelines become outdated within 5.8 years of publication, and only 78% of recommendations remain valid at 4 years. This creates compliance risks and patient safety concerns when staff unknowingly follow superseded protocols.
These aren't abstract risks. As many as 1 in 10 hospitalized patients experiences harm, with nearly 50% of adverse events considered preventable. Communication and information gaps are among the most documented contributors to those preventable events.
The Joint Commission's 2024 sentinel event data makes the connection concrete: 47% of delay-in-treatment events were tied to failures to recognize or respond to changes in patient condition — exactly the scenarios where timely access to the right protocol matters most.

What AI Makes Possible in Healthcare KM Today
Semantic Search Beyond Keywords
AI-powered search understands query intent, not just exact term matches. When a nurse asks "post-op wound care for diabetic patients," semantic search delivers precise, contextual guidance rather than a generic list of documents requiring manual triage. This matters because physicians generate approximately 5.5 clinical questions per half-day observation period but don't pursue answers to 45% of those questions, primarily due to time constraints. Legacy keyword search that returns unranked, unfiltered results makes the problem worse.
Natural language processing (NLP) transforms unstructured clinical text into structured, usable knowledge. Incorporating NLP-derived keywords into clinical prediction models increased prediction accuracy from 83.1% to 92.2% in ICU mortality studies, demonstrating the value of semantic processing.
Healthcare staff can query in conversational language and receive answers drawn from medical literature, organizational protocols, and verified knowledge bases — no specialized search syntax required.
AI-Assisted Content Creation and Maintenance
AI authoring tools allow knowledge managers to draft, rephrase, summarize, and translate clinical content at scale. What once took hours now happens in minutes. These tools reduce the time required to publish or update protocols, helping organizations stay current as clinical guidelines and protocols change.
Auto-translation into 15+ languages supports multilingual healthcare workforces — a critical capability when approximately 27.5 million U.S. residents have limited English proficiency, nearly 1 in 10.
AI summarization condenses lengthy clinical articles into digestible formats, while rephrasing tools adjust tone and clarity for different audiences. The maker-checker approval process ensures clinical validation before content goes live, maintaining accuracy while accelerating publication cycles.
Automated Knowledge Gap Detection
AI analyzes how staff interact with knowledge bases — identifying unanswered queries, low-engagement content, and escalation patterns. This proactive approach flags gaps before they cause errors or delays. The underlying mechanism: micro-segmented analytics that track time spent on content, user feedback, and failed searches, surfacing patterns that reveal where knowledge resources fall short.
For example, if multiple agents escalate insurance eligibility questions, the system flags this as a content gap requiring new decision trees or FAQs. Over time, this feedback loop means the knowledge base reflects how staff actually work — not how administrators assumed they would.
Guided Decision Trees for Complex Workflows
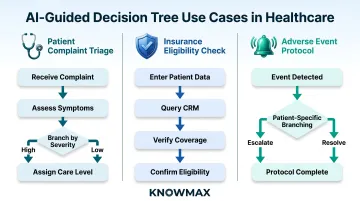
AI-powered decision trees walk staff through multi-step, conditional processes without relying on memorization:
- Patient complaint triage — step-by-step assessment ensuring no critical symptom is overlooked
- Insurance eligibility checks — guided workflows that integrate with CRM systems to verify coverage in real time
- Adverse event protocols — conditional branching that adapts based on patient-specific data
These workflows integrate with existing systems via APIs, fetching patient data to personalize each interaction. The result: faster resolutions, improved compliance, and reduced cognitive burden on staff navigating complex clinical or administrative scenarios.
Real-Time Knowledge Updates with Proactive Alerts
AI-enabled platforms push protocol updates to staff when changes occur — rather than waiting for someone to stumble upon the new version. Updates can be delivered via email, Slack, Microsoft Teams, or tickers within the knowledge platform itself. Staff acknowledge receipt, creating an audit trail that documents who saw what information and when.
This capability is critical in healthcare, where using outdated protocols can have serious consequences. Real-time alerts ensure the entire organization operates from the current source of truth, reducing lag time between policy changes and frontline implementation.
AI-Powered Knowledge Delivery Across the Healthcare Ecosystem
Clinical Staff at the Point of Care
AI surfaces relevant protocols, drug interaction checks, and care pathway guidance directly within clinical workflows. Integration with EHR systems means clinicians access knowledge without exiting their primary interface, reducing cognitive burden and enabling faster decisions at the point of care.
Role-based access ensures physicians, nurses, and specialists see only information relevant to their scope of practice.
Healthcare Contact Center and Support Teams
Agents handling insurance queries, appointment scheduling, or medication questions benefit from AI-guided knowledge delivery that:
- Reduces average handling time through instant access to verified answers
- Improves first-contact resolution by surfacing complete information upfront
- Ensures consistent answers across phone, email, chat, and portal channels
HIPAA-certified platforms like Knowmax give healthcare contact centers access to AI-powered search, decision trees, and guided workflows — so agents apply the same verified protocols that clinical teams use, without switching between systems.
Administrative and Operational Staff
Billing teams, intake coordinators, and compliance officers benefit from AI-powered KM that keeps them current with:
- Latest payer policies and reimbursement rules
- HIPAA requirements and facility-specific procedures
- Regulatory changes affecting documentation or reporting
This eliminates constant manual research and reduces administrative errors that lead to claim denials or compliance issues.
Patient Self-Service and Digital Channels
AI-powered knowledge bases surface accurate, approved information to patients via chatbots, portals, and IVR systems. Patients independently access information about:
- Appointment scheduling and management
- Insurance benefits and prior authorizations
- Post-care instructions and medication guidance
- Test results and medical records
The result: fewer inbound contacts and patients who find verified answers on their own, at any hour.
Cross-Departmental Consistency
AI ensures all roles — from ICU nurses to billing coordinators to call center agents — operate from the same verified knowledge base. This matters because siloed systems routinely cause different departments to give conflicting information, each referencing a different source. A unified knowledge layer closes that gap across every channel and team.
Measurable Benefits of AI-Driven Healthcare KM
Reduced Medical and Administrative Errors
AI surfaces the right protocol at the right moment, reducing reliance on memory or outdated documents. The mechanism is straightforward: when staff have instant access to current, contextual guidance, they make fewer mistakes. Annual costs of preventable adverse events in hospitalized patients are estimated at $17.1 billion in direct healthcare costs, with total social costs approaching $950 billion. Even incremental improvements in knowledge accessibility yield measurable ROI.
Globally, medication errors alone cost an estimated $42 billion annually, approximately 1% of global health expenditure. Better knowledge management directly addresses this problem by ensuring staff reference current drug interaction databases, dosing protocols, and administration guidelines.

Faster Onboarding and Continuous Training
AI-powered KM compresses onboarding timelines by giving new staff immediate access to structured, searchable knowledge rather than relying on shadowing or manual training packets. The average cost of turnover for a single bedside RN is $61,110, with hospitals losing $3.9M to $5.7M annually to nurse turnover. It takes approximately 3 months to fill a clinical role. Faster onboarding reduces vacancy costs and gets new staff productive sooner.
Modern AI-powered KM platforms support this through:
- Structured learning paths tailored to clinical and support roles
- Gamified training modules that accelerate protocol mastery
- AI-generated assessments with instant feedback
- Gap identification that triggers targeted remediation automatically
Improved Compliance and Audit Readiness
AI-maintained knowledge bases with version control, update logs, and role-based access create a traceable record of what information staff had access to and when. This directly supports HIPAA compliance audits and Joint Commission readiness. Scheduled content availability ensures outdated protocols automatically expire, preventing accidental use of superseded guidelines.
Archiving capabilities preserve historical versions for audit purposes without cluttering active workflows — so inspectors can pull a specific protocol version from 18 months ago without any manual digging.
Better Patient Outcomes and Satisfaction
Upstream improvements — accurate protocols, consistent information delivery, faster resolutions — translate to downstream patient experience gains. Patients who reported that nurses "always" listened carefully to them had 18% lower odds of 30-day readmission. Patients who reported that doctors "always" explained things clearly had 18% lower readmission odds.
Better knowledge management supports both outcomes by ensuring staff have the information needed to communicate clearly and make informed decisions. HCAHPS scores account for 30% of total Value-Based Purchasing scores, affecting up to 2% of financial reimbursements. For a 500-bed hospital, that 2% swing can represent millions in annual reimbursement.
Challenges and Considerations When Adopting AI in Healthcare KM
Accuracy, Hallucination Risk, and Clinical Validation
AI-generated or AI-retrieved content must be validated by subject matter experts before deployment in clinical or patient-facing contexts. Hallucination risk — where AI confidently presents incorrect information — is unacceptable in healthcare. Organizations need human-in-the-loop review workflows and clear governance policies for knowledge approval and update cycles.
Platforms should support maker-checker processes where clinical leads validate content before publication. This combines AI's speed with expert oversight, maintaining accuracy while accelerating content cycles.
HIPAA Compliance and Data Security
Any AI-powered KM platform deployed in healthcare must meet strict data security standards:
- HIPAA — Requires Business Associate Agreements with all cloud vendors handling ePHI; providers carry direct liability under HIPAA Rules
- SOC 2 — Covers security, availability, processing integrity, confidentiality, and privacy — a baseline expectation for enterprise healthcare vendors
- ISO 27001 — Certifies a structured, auditable information security management system

Organizations should evaluate vendors on security certifications, role-based access controls, audit trail capabilities, and encryption standards. HHS requires Business Associate Agreements with all cloud service providers handling ePHI, with direct liability under HIPAA Rules.
Change Management and Cultural Adoption
Shifting from email-based or siloed knowledge habits to a centralized AI-powered system requires leadership buy-in, training, and a culture that rewards knowledge contribution. 80% of healthcare providers cite time pressures as the primary barrier to pursuing clinical answers, and 55% report they don't know what a clinical decision support tool is.
These numbers point to a harder truth: technical implementation is often easier than sustainable adoption. Staff need a platform intuitive enough that they choose it over familiar workarounds. Success factors include:
- Executive sponsorship and visible leadership support
- Integration with existing workflows to minimize disruption
- User-centered design that matches staff mental models
- Ongoing training and support during transition periods
The Joint Commission and Coalition for Health AI released guidance on responsible AI use in healthcare in September 2025, recommending internal governance, local validation of AI tools, continuous monitoring, and flexible integration. With voluntary AI certification planned for 2026, organizations that build governance frameworks today will be better positioned — both for compliance and for staff trust in the tools they use.
Frequently Asked Questions
What are the 5 pillars of healthcare knowledge management?
The five pillars are People, Processes, Content, Technology, and Culture. People create and use knowledge; Processes govern how knowledge flows; Content is the information itself; Technology enables storage and delivery; Culture determines whether knowledge sharing is valued and rewarded.
What are the 5 C's of healthcare knowledge management?
The 5 C's are Creation, Conversion, Communication, Change, and Compliance. They map the knowledge lifecycle — from generating information and converting it into usable formats, to communicating it to users, adapting it as circumstances evolve, and keeping it aligned with regulatory requirements.
What are the 5 P's of healthcare knowledge management?
The 5 P's are Purpose, People, Process, Platform, and Performance. Together, they cover the strategic dimensions healthcare organizations must align — from defining why KM matters and engaging the right stakeholders, to selecting technology and measuring outcomes.
What are the 4 pillars of healthcare knowledge management?
The 4-pillar model includes Knowledge Creation, Knowledge Storage, Knowledge Sharing, and Knowledge Application. Creation and Storage handle how knowledge is authored and organized; Sharing and Application determine how it reaches staff and drives better care decisions.
How does AI specifically improve knowledge management in healthcare?
AI improves healthcare KM through semantic search that understands query intent, automated content maintenance that keeps protocols current, guided decision trees that ensure process compliance, and proactive knowledge delivery that pushes updates to staff when changes occur — so staff spend less time searching and more time acting on accurate information.
Is AI-powered healthcare knowledge management HIPAA compliant?
HIPAA compliance is determined by the platform's security architecture, not the AI layer. Organizations should select vendors with HIPAA, SOC 2, and ISO 27001 certifications, Business Associate Agreements, role-based access controls, audit trail capabilities, and encryption for data at rest and in transit.


